#1 Affordable Medical Billing Services in USA
Healthcare Claims Processing in : How It Works, Challenges, and Solution
Accurate claims processing is the backbone of a healthy revenue cycle.
In this guide, we break down everything you need to know about medical claims processing and how the right support can help your practice get paid faster with fewer denials


What is Medical Claims Processing?
Claims Processing Services involve the processing and management of health insurance claims from submission to resolution. Claims processing service providers can improve claim turnaround times and increase the accuracy of claims adjudication. These providers efficiently handle the verification and validation of claims, ensuring higher accuracy and timely payouts. Claims BPO services are one of the fastest ways to leverage automation and AI in claims processing management.
Insurance companies, healthcare providers, and many other organizations rely on Claims Processing Services to improve insurance claims processing efficiency. By outsourcing claims processing, businesses can access the expertise and technology offered by service providers to reduce operational costs and speed up claim handling.
How Claims Processing Works
PractiAssist provides end-to-end insurance workflow by handling verification, eligibility checks, claims submission, and follow-ups in one system. It reduces delays and errors by using trained VAs + automation to ensure faster approvals and smoother reimbursements from start to finish.
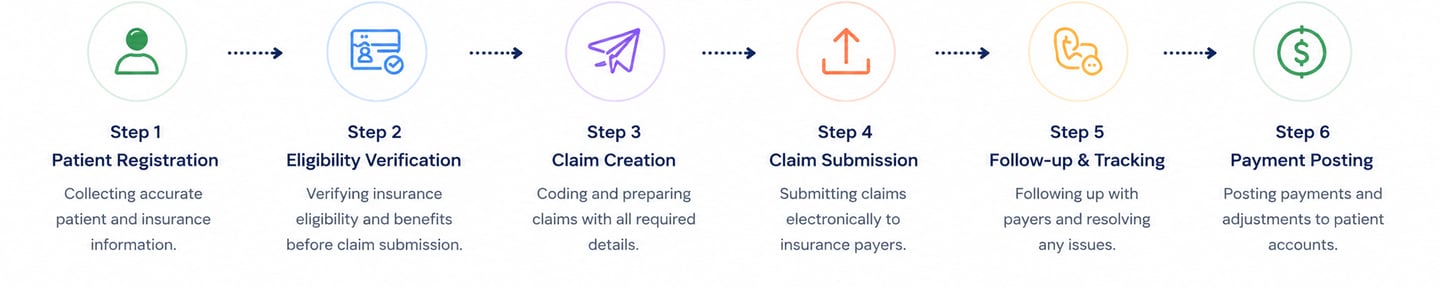
Common Challenges in Medical Claims Processing
Even the most experienced in-house teams face challenges. Complex payer requirements, frequent policy updates, and high claim volumes can slow down the process and impact collections.
High denial rates: Errors in coding, missing information, or eligibility issues lead to rejections.
Delayed reimbursements: Slow follow-ups and inefficient tracking extend payment cycles.
Complex payer rules: Every insurance company has different requirements and policies.
Coding and data errors: Incorrect codes or incomplete data can cause claim rejections.
Time-consuming follow-ups: Manual follow-ups take valuable time away from patient care.
Revenue leakage: Unresolved denials and underpayments impact overall revenue.




Claim Errors Are
Costing You More
Than You Think
Even small mistakes in claims submission can lead to denied claims, delayed payments, and lost revenue.
☑️ Denied claims slow down your cash flow
☑️ Fixing errors takes hours of your time
☑️ Some revenue is never recovered
That’s Where PractiAssist Comes In
Our medical claims specialists ensure your claims are clean, accurate, and submitted on time—so you get reimbursed faster with fewer denials.
Discover what PractiAssist can do for you and your Practice
Tell us more & we will contact you within 24 hours




Support
Drop an email/call us and we'll get back to you as soon as possible:
About Practiassist
Contact
© 2024. All rights reserved.
Email: practiassist@gmail.com
Phone: +1 (201) 355 4450




